Category: heart-disease

This post is courtesy of a mentor, forever instructor (Functional Medicine University), and an example of what healthcare should be, Dr. Ronald Grisanti D.C., D.A.B.C.O., D.A.C.B.N. M.S. As a reader Read More

Brainwashing works. It’s also really hard to unlearn. It’s amazing how many conversations I have with potential new clients that are either worried or excited about their cardiac health based Read More

Arthritis can be debilitating. In fact, arthritis and rheumatoid conditions are the leading cause of disability among US adults for the past 15 years. So when your doctor is assessing your Read More

This post is for all those fatties out there. You know who I’m talking about…fatty, fatty, fat, fat. Yeah, I called you fat, look at me I’m skinny. Never stopped me Read More

If you are being treated for high blood pressure, I’m sure you’ve been told to watch your sodium intake. The traditional medical theory is that since you consume too much Read More

If you were a child of the 80s and 90s like myself, you will remember this commercial. “This is your brain. This is drugs. This is your brain on drugs. Read More

This is more of a ‘random thoughts’ post. It’s not lengthy, but hopefully one to get you thinking a bit differently about heart disease and a way to improve your risk Read More

I have a number of pet peeves. For those that know me really well, you know I can go from zero to maximum irritability in 0.2 seconds when I see random Read More

Breakfast vs. Dessert On my initial intake paperwork for people, I have the potential client list out their food items. Under more investigation of the ingredients of those foods, I Read More
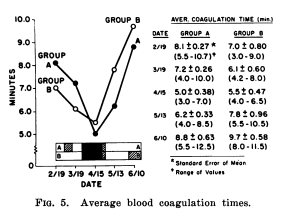
A friend of mine passed an article to me from The Wall Street Journal. It was an article about how stress raises cholesterol. My initial mental reaction was, ‘Duh, what Read More
If you’ve been reading for a while, you know I harp on inflammation a lot. I’ve mentioned inflammation coming from the immune system, your belly fat, and even your liver. Read More

Fat and Fabulous I was giving a presentation to a group of other doctors and students in the mental health field last week. One attendee interrupted me when I was Read More
You may not have heard of some recent news that is happening across the pond in the mother country concerning taking statins. You know statins as those drugs that are Read More

It’s February and with no surprise, the media is all over ‘heart disease’ awareness campaigns. But if you keep following what the media (and your doctor) push, you will probably Read More
